Gene therapy success raises hopes of 'cure' for HIV
Doctors say engineering an HIV patient's own immune cells could eliminate the need for daily antiretroviral drugs
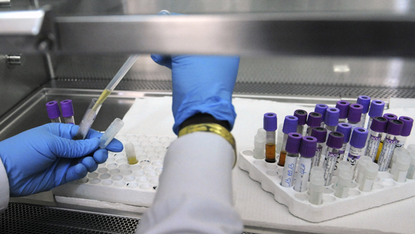
DOCTORS have used gene therapy to modify the immune systems of 12 patients to help "shield" them from the effects of HIV, the BBC reports.
The new treatment could replace programmes that require HIV patients to take antiretroviral medication every day.
In a study published in the New England Journal of Medicine on Wednesday, scientists said that by creating beneficial mutations in T-cells they might have found a new therapy for improving the health of people with HIV.
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
Some patients have a rare mutation in their T-cells, white blood cells that are vital to human immune responses, that prevents the virus from getting inside and multiplying.
Doctors working on the study reported that patients receiving their genome-modifying treatment had "decreased viral loads". In one patient who had received the treatment the virus could no longer be detected at all.
Out of the 12 people who took part in the test, six stopped taking their antiretroviral medication so that researchers could assess the effects of the genome-modifying treatment. In four of those patients, the amount of HIV in the blood dropped. And in one patient, the virus could "no longer be detected at all", according to a Massachusetts Institute of Technology (MIT) report.
Doctors stressed that the study was only intended to determine the safety of the treatment, rather than determining whether "HIV shielding" could be a feasible replacement for drug treatment.
"We are absolutely encouraged by these results," said Bruce Levine the director of the Clinical Cell and Vaccine Production Facility at the University of Pennsylvania. "It is an evolution in the treatment of HIV from daily antiretroviral therapy."
Levine, who ran the study with his colleague Carl June, noted that it was too early to say whether the treatment could come to replace daily antiretroviral drugs, The Guardian reports.
"Cure is a four letter word. We don't like to use it, particularly with HIV. We are looking at improving the health and immune function of people with HIV," Levine said.
Academics cautiously welcomed the findings. In an editorial that sat alongside the report, researchers from Stanford and Harvard Universities, Mark Kay and Bruce Walker, wrote: "The tantalising question... is whether it might actually have been partially effective. A definitive answer to this question will require additional studies."
Create an account with the same email registered to your subscription to unlock access.
Sign up for Today's Best Articles in your inbox
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
 'Make legal immigration a more plausible option'
'Make legal immigration a more plausible option'Instant Opinion Opinion, comment and editorials of the day
By Harold Maass, The Week US Published
-
 LA-to-Las Vegas high-speed rail line breaks ground
LA-to-Las Vegas high-speed rail line breaks groundSpeed Read The railway will be ready as soon as 2028
By Peter Weber, The Week US Published
-
 Israel's military intelligence chief resigns
Israel's military intelligence chief resignsSpeed Read Maj. Gen. Aharon Haliva is the first leader to quit for failing to prevent the Hamas attack in October
By Justin Klawans, The Week US Published
-
 Home Office worker accused of spiking mistress’s drink with abortion drug
Home Office worker accused of spiking mistress’s drink with abortion drugSpeed Read Darren Burke had failed to convince his girlfriend to terminate pregnancy
By The Week Staff Published
-
 In hock to Moscow: exploring Germany’s woeful energy policy
In hock to Moscow: exploring Germany’s woeful energy policySpeed Read Don’t expect Berlin to wean itself off Russian gas any time soon
By The Week Staff Published
-
 Were Covid restrictions dropped too soon?
Were Covid restrictions dropped too soon?Speed Read ‘Living with Covid’ is already proving problematic – just look at the travel chaos this week
By The Week Staff Last updated
-
 Inclusive Britain: a new strategy for tackling racism in the UK
Inclusive Britain: a new strategy for tackling racism in the UKSpeed Read Government has revealed action plan setting out 74 steps that ministers will take
By The Week Staff Published
-
 Sandy Hook families vs. Remington: a small victory over the gunmakers
Sandy Hook families vs. Remington: a small victory over the gunmakersSpeed Read Last week the families settled a lawsuit for $73m against the manufacturer
By The Week Staff Published
-
 Farmers vs. walkers: the battle over ‘Britain’s green and pleasant land’
Farmers vs. walkers: the battle over ‘Britain’s green and pleasant land’Speed Read Updated Countryside Code tells farmers: ‘be nice, say hello, share the space’
By The Week Staff Published
-
 Motherhood: why are we putting it off?
Motherhood: why are we putting it off?Speed Read Stats show around 50% of women in England and Wales now don’t have children by 30
By The Week Staff Published
-
 Tonga’s tsunami: the aid effort turns political
Tonga’s tsunami: the aid effort turns politicalSpeed Read Efforts to help Tonga’s 105,000 residents have been beset by problems
By The Week Staff Published