Lasting impact: how Covid damages the human brain
New research suggests coronavirus complications may include stroke and psychosis
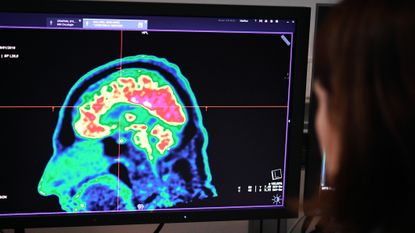
Doctors have repeatedly warned that coronavirus patients may be left with life-altering health problems - and now new research has shone a light on the threat posed to the body’s most vital organ.
Brain complications including stroke and psychosis have been linked to Covid-19 in a study “that raises concerns about the potentially extensive impact of the disease in some patients”, The Guardian reports.
Experts say the findings “highlight the need to investigate the possible effects of Covid-19 in the brain and studies to explore potential treatments”, the newspaper adds.
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
Covid and the brain
The study, published in The Lancet, looked in detail at 125 “severe cases” of Covid in the UK. The data was collected between 2 April and April 26, “when the disease was spreading exponentially” across the country, says The Telegraph.
The most common brain-related complication seen was stroke, which was recorded in 77 of the patients. Most of those affected were over 60 years old, and the strokes were ischaemic - caused by a blood clot in the brain.
In the remaining stroke cases, nine patients had a brain haemorrhage, and one had a stroke caused by inflammation in the blood vessels of the brain. Covid has previously been found to “cause severe inflammation and blood clots in the lungs and elsewhere in the body”, The Guardian reports.
As well as strokes, the study found that a number of the patients experienced “confusion or changes in behaviour reflecting an altered mental state”. Seven of these patients were also found to have suffered inflammation of the brain, known as encephalitis.
The patients with altered mental states were later diagnosed with a range of psychiatric conditions including psychosis, a dementia-like syndrome and mood disorders.
A first in the field?
While the newly published study is one of the largest yet on brain complications and Covid, scientists have been hinting at a possible link since the early days of the pandemic.
In March, medics at Strasbourg University Hospital in northeast France reported that in some severe Covid cases, patients appeared to be “extremely agitated” and were experiencing “neurological problems” including “confusion and delirium”.
Julie Helms, a doctor at the hospital, told the BBC that “we are used to having some patients in the ICU who are agitated and require sedation, but this was completely abnormal”.
“It has been very scary, especially because many of the people we treated were very young – many in their 30s and 40s, even an 18-year-old,” she added.
Helms’ team reported their findings in the New England Journal of Medicine, describing signs of “encephalopathy”, the general medical term for damage to the brain.
Signs of brain damage in coronavirus patients had also been noted back in February by researchers in Wuhan, the Chinese city at the centre of the global outbreak.
Earlier this month, the Financial Times reported that researchers at Johns Hopkins University in Baltimore had found “the first direct evidence that coronavirus could infect the human brain and replicate inside its cells”.
In tests, the scientists added low levels of Sars-Cov-2, the virus that causes the disease, to “tiny neuronal balls known as mini-brains that are grown from human stem cells”, says the newspaper. They observed how the “virus infected neurons in the mini-brains… [and] then multiplied within the neurons”.
Within three days, the study found the number of copies of the original Covid virus had increased “at least tenfold”.
According to the BBC, more than 300 studies across the globe have found “a prevalence of neurological abnormalities in Covid-19 patients”. The extent of the problem remains unclear, but experts estimate that “roughly 50% of patients diagnosed with Sars-CoV-2... have experienced neurological problems”, says the broadcaster.
–––––––––––––––––––––––––––––––For a round-up of the most important stories from around the world - and a concise, refreshing and balanced take on the week’s news agenda - try The Week magazine. Start your trial subscription today –––––––––––––––––––––––––––––––
So what happens next?
Sarah Pett, who co-led the new study, says that while the findings are not conclusive, the research forms an “important snapshot of the brain-related complications of Covid-19 in hospitalised patients”.
“It is critically important that we continue to collect this information to really understand this virus fully,” added Pett, a lecturer in infectious disease at University College London.
That call has been echoed by other scientists.
Michael Sharpe, a professor of psychological medicine at the University of Oxford, said that the report “reminds us that Covid-19 is more than a respiratory infection and that we need to consider its link to a variety of other illnesses”.
However, “people in the general population should not worry too much about these possibly associated illnesses as they are probably relatively rare”, he added.
Emphasising that point, study co-leader Benedict Michael, a senior clinician scientist fellow at Liverpool University, “said it was important to note that the study focused on severe cases”, The Telegraph reports.
But Michael noted that the research was an important step towards defining Covid-19’s effect on the brain, adding that “we now need detailed studies to understand the possible biological mechanisms ... so we can explore potential treatments”.
Create an account with the same email registered to your subscription to unlock access.
Sign up for Today's Best Articles in your inbox
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
 Today's political cartoons - April 20, 2024
Today's political cartoons - April 20, 2024Cartoons Saturday's cartoons - papal ideas, high-powered debates, and more
By The Week US Published
-
 5 sleeper hit cartoons about Trump's struggles to stay awake in court
5 sleeper hit cartoons about Trump's struggles to stay awake in courtCartoons Artists take on courtroom tranquility, war on wokeness, and more
By The Week US Published
-
 The true story of Feud: Capote vs. The Swans
The true story of Feud: Capote vs. The SwansIn depth The writer's fall from grace with his high-flying socialite friends in 1960s Manhattan is captured in a new Disney+ series
By Adrienne Wyper, The Week UK Published
-
 Covid four years on: have we got over the pandemic?
Covid four years on: have we got over the pandemic?Today's Big Question Brits suffering from both lockdown nostalgia and collective trauma that refuses to go away
By Chas Newkey-Burden, The Week UK Published
-
 The hollow classroom
The hollow classroomOpinion Remote school let kids down. It will take much more than extra tutoring for kids to recover.
By Mark Gimein Published
-
 How love impacts your health
How love impacts your healthThe Explainer Turns out you actually can die of a broken heart
By Devika Rao, The Week US Published
-
 Martha's Rule: patients given right to urgent second opinion
Martha's Rule: patients given right to urgent second opinionThe Explainer Hospitals in England will launch new scheme that will allow access to a rapid treatment review
By Richard Windsor, The Week UK Published
-
 The contaminated blood scandal
The contaminated blood scandalThe Explainer Widely regarded as the worst treatment disaster in the history of the NHS, the public inquiry is due to publish its report in May
By The Week UK Published
-
 How helpful are mental health apps?
How helpful are mental health apps?Under the radar Market is booming, offering accessibility and affordability, but many apps are unregulated and share sensitive user data
By Harriet Marsden, The Week UK Published
-
 Can Britain's dental crisis be fixed?
Can Britain's dental crisis be fixed?The Explainer New proposals include more money for dentists working in under-served areas
By Richard Windsor, The Week UK Published
-
 Excess screen time is making children only see what is in front of them
Excess screen time is making children only see what is in front of themUnder the radar The future is looking blurry. And very nearsighted.
By Devika Rao, The Week US Published