Coronavirus: inside the ‘ten-month marathon’ to produce Oxford vaccine
Team behind university’s Covid jab admit the 90% effective dosage was discovered by mistake
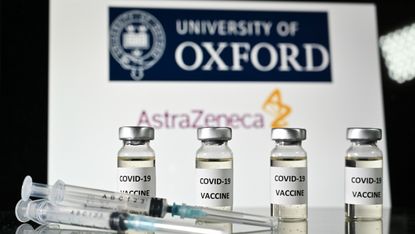
While most of the world descended into panic when the coronavirus pandemic first emerged, a group of scientists at Oxford University were springing into action to develop a vaccine to fight Covid-19.
Although late-stage trials indicate that competing vaccines from Pfizer and Moderna are slightly more effective, the Oxford jab has been heralded as a potential game-changer thanks to its ease of storage and lower price tag.
As countries including the UK now line up to reserve millions of doses, the director of the Oxford Vaccine Group, Andrew Pollard, said: “We have a vaccine for the world... this is an incredibly exciting moment for human health.”
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
Lesson in team work
The Oxford vaccine’s origin can be traced back to a meeting of the university’s academics in early February. “In China, a new virus was spreading rapidly. Soon it would be here,” says The Times. “This was it: the ‘disease X situation’.”
Following the meeting, Sarah Gilbert, a professor of vaccinology at the university’s Jenner Institute, was put in charge of the scientists tasked with creating a vaccine to combat the then unknown virus.
The formation of the research team would set in motion what the newspaper describes as a “ten-month coronavirus marathon”.
“We had recently started thinking about an appropriate response to Disease X - how could we mobilise and focus our resources to go more quickly than we had ever gone before,” Gilbert recalls. “And then Disease X arrived.”
Also in that initial meeting with her were “Adrian Hill, a colleague in the Jenner vaccine institute, and Andrew Pollard, who had no academic expertise in the vaccine platform”, The Times reports. “His expertise, instead, was in something in its own way just as fiendishly complex: running large-scale clinical trials.”
How the jab was developed
In March, as the severity of the outbreak became increasingly apparent, Gilbert’s team was awarded a £2.2m grant from the UK’s National Institute for Health Research and the UK Research and Innovation funding agency.
This financial backing allowed Gilbert “to scale up her team’s efforts to move into coronavirus disease 2019 vaccine preclinical and clinical trials”, as The Lancet reported the following month.
Her team were also granted ethical approval for a clinical trial and conditional approval from the UK Medicines and Healthcare products Regulatory Agency to screen volunteers for trial enrolment.
“Ideally, we need the clinical trial to be taking place when the majority of volunteers have not been exposed to the virus,” Gilbert told The Lancet. “We will exclude volunteers who have a positive PCR test for Sars-CoV-2, or who have had fever or cough in the past month.”
After animal trials had shown that the vaccine was safe, the researchers began human trials on 23 April. A week later, the team partnered with Cambridge-based pharmaceutical giant AstraZeneca to enable mass production and rollout of the vaccine if the trials proved successful.
Trials and tribulations
The testing process for the Oxford jab was split into the usual three phases designated for clinical vaccine trials.
In Phase 1, the vaccine is tested on a small number of people to check whether it is safe. This is followed by a Phase 2 trial in which more more people are tested, and then Phase 3, which the BBC describes as “the big trial, involving thousands of people, to prove it actually protects people”.
The Oxford vaccine has now completed all three stages, with a total of 30,000 volunteers in the UK, US, Brazil and South Africa tested in Phase 3.
These final-stage trials found that the vaccine had an overall efficacy of 70.4%. But this rose to 90% among trial participants given a half dose followed by a full dose a month later, as opposed to the standard two full doses.
The more effective dosage level was discovered by chance, after the initial half doses was administered as a result of an error.
“The reason we had the half dose is serendipity,” Mene Pangalos, executive vice-president of biopharmaceuticals research and development at AstraZeneca, told The Guardian.
After noticing that side-effects were reduced in some trial candidates, “we went back and checked… and we found out that they had underpredicted the dose of the vaccine by half,” Pangalos said. Rather than restarting the trial, the researchers decided to push ahead and administer the full dose booster as scheduled.
It is not currently known why administering a half dose first makes the vaccine more effective.
Science journal Nature notes that the Oxford version is designed to trigger “an immune response not only to the Sars-CoV-2 spike protein, but also to components of the viral vector”. Some experts have suggested that if the first dose is administered in full, it “blunts” this reaction, making the vaccine less effective overall.
PR battle
The UK government has pre-ordered 100 million doses of the Oxford vaccine, and AstraZeneca has pledged to make a total of three billion doses for global distribution next year.
But “now that it looks like we will have a vaccine sooner rather than later, it’s becoming clear that the PR and comms surrounding it could be just as important as the logistics of distribution”, says Wired.
The next key step is to reassure “ordinary members of the public that the vaccine is safe”, and to reach out “to those who are reluctant to take it, either because of health concerns, or because they’ve been drawn into the vortex of fake news”, the magazine continues.
The importance of this PR push has been emphasised by Heidi Larson, director of the Vaccine Confidence Project.
“We need to bring the public along on the journey,” she says. “We’re at a very low trust level with our populations more broadly, and they don’t just want to know how good the product is, they want to know about the process.
“Now is the time to talk about the process, and deciding who gets it first and why.”
Create an account with the same email registered to your subscription to unlock access.
Sign up for Today's Best Articles in your inbox
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
 Major League Baseball is facing an epidemic of pitcher's injuries
Major League Baseball is facing an epidemic of pitcher's injuriesUnder the Radar Many insiders are blaming the pitch clock for the rise in injuries — but the league is not so sure
By Justin Klawans, The Week US Published
-
 8 movie musicals that prove the screen can share the stage
8 movie musicals that prove the screen can share the stageThe Week Recommends The singing and dancing, bigger than life itself
By Scott Hocker, The Week US Published
-
2024 Mother's Day Gift Guide
The Week Recommends A present for every mom
By Catherine Garcia, The Week US Published
-
 Covid four years on: have we got over the pandemic?
Covid four years on: have we got over the pandemic?Today's Big Question Brits suffering from both lockdown nostalgia and collective trauma that refuses to go away
By Chas Newkey-Burden, The Week UK Published
-
 The hollow classroom
The hollow classroomOpinion Remote school let kids down. It will take much more than extra tutoring for kids to recover.
By Mark Gimein Published
-
 Excess screen time is making children only see what is in front of them
Excess screen time is making children only see what is in front of themUnder the radar The future is looking blurry. And very nearsighted.
By Devika Rao, The Week US Published
-
 Covid-19: what to know about UK's new Juno and Pirola variants
Covid-19: what to know about UK's new Juno and Pirola variantsin depth Rapidly spreading new JN.1 strain is 'yet another reminder that the pandemic is far from over'
By Arion McNicoll, The Week UK Published
-
 Long-term respiratory illness is here to stay
Long-term respiratory illness is here to stayThe Explainer Covid is not the only disease with a long version
By Devika Rao, The Week US Published
-
 Covid inquiry: the most important questions for Boris Johnson
Covid inquiry: the most important questions for Boris JohnsonTalking Point Former PM has faced weeks of heavy criticism from former colleagues at the public hearing
By The Week Staff Published
-
 China's pneumonia cases: should we be worried?
China's pneumonia cases: should we be worried?The Explainer Experts warn against pushing 'pandemic panic button' following outbreak of respiratory illness
By Keumars Afifi-Sabet, The Week UK Published
-
 Vallance diaries: Boris Johnson 'bamboozled' by Covid science
Vallance diaries: Boris Johnson 'bamboozled' by Covid scienceSpeed Read Then PM struggled to get his head around key terms and stats, chief scientific advisor claims
By The Week UK Published