Malaria vaccine given green light by EU regulators
Mosquirix gets European approval to be used on African babies to help control impact of malaria
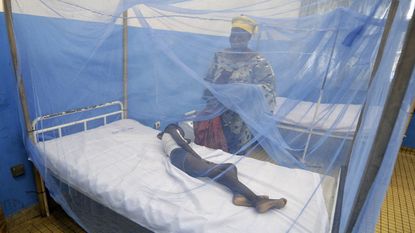
The world's first malaria vaccine has earned the approval of European drug regulators, who say it should be licensed for use in Africa, where babies are at risk of contracting the disease.
The RTS,S shot, known as Mosquitrix, took 30 years to develop and would be the first-ever licensed vaccine against human parasites, Al Jazeera reports. British drugmaker GlaxoSmithKline (GSK) developed the drug in partnership with the PATH Malaria Vaccine Initiative, with funding from the Bill & Melinda Gates Foundation.
Malaria killed an estimated 584,000 people in 2013, the vast majority of them in sub-Saharan Africa. More than 80 per cent of those deaths were of children under age five.
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
GSK CEO Andrew Witty is optimistic about the impact of Mosquitrix, but acknowledged that his company's drug is not a cure-all solution.
"While RTS,S on its own is not the complete answer to malaria, its use alongside those interventions currently available such as bed nets and insecticides would provide a very meaningful contribution to controlling the impact of malaria," he said.
Trial data released in 2011 and 2012 showed the drug only reduced episodes of malaria in babies aged six- to 12-weeks by 27 per cent, and by around 46 per cent in children aged five- to 17-months.
Nonetheless, the European Medicines Agency (EMA) recommends that the drug be licensed for administration to the full age range of study participants – from six weeks to 17 months. The European Commission normally ratifies EMA recommendations within several months.
The drug will now be assessed by the World Health Organization (WHO) and will have to be reviewed by national regulatory authorities in any country wishing to use it. The WHO suggests it is therefore unlikely to be rolled out until at least 2017.
Specialists expressed concerns over the partial efficacy of the drug, and questioned whether the benefits of vaccination outweigh the cost of vaccinating the countless children in need.
But Joe Cohen, a GSK scientist who has led the development of Mosquitrix since 1987, said he has "absolutely no reservations in terms of rolling this vaccine out... It will have an enormously significant public health impact."
Malaria vaccine only partially effective but still a 'breakthrough'
24 April
The world's first malaria vaccine has been hailed as an important step in eradicating the disease, despite only being partially effective.
British drug manufacturer GlaxoSmithKline has been developing the RTS,S vaccine for over two decades, but observers argue there is still a long way to go.
Tests on 16,000 children from seven African countries revealed that the vaccine's ability to protect children gradually waned over time, and booster doses were not always effective. It was also not effective in young babies and had unexplained side effects, but researchers say it could still reduce human infections by 30 per cent, saving countless lives.
Roughly 1,300 children in sub-Saharan Africa die from malaria every day. "Preventing some of those attacks is not insignificant," the study's author Brian Greenwood told Sky News.
"Everyone accepts that this is not the perfect or the last malaria vaccine," he said. "It's not good enough to stop transmission but it will cut the huge burden of disease."
The reason the vaccine was not as effective as scientists had hoped was because the malaria parasite has a complicated life cycle and has evolved to evade the human immune system over hundreds of years, the BBC explains.
Side-effects of the vaccine included pain, fever and convulsions, as well as a higher rate of meningitis, something scientists were unable to explain.
The University of Oxford's Professor Adrian Hill said he had additional concerns about the drug. "More worrying is the new evidence of a rebound in malaria susceptibility: after 20 months, vaccinated children who were not boosted showed an increased risk of severe malaria to non-vaccinated controls."
But James Whiting, from the charity Malaria No More UK, said just getting the vaccine this far was a significant achievement.
"There are still a number of considerations and approval processes to be undertaken, but it has the potential to be an important additional tool to fight malaria and save lives from a disease that kills a child every minute."
The European Medicines Agency will now meet to analyse the data and decide whether to licence the drug, and The World Health Organization will then make a decision on whether or not to recommend its use.
Create an account with the same email registered to your subscription to unlock access.
Sign up for Today's Best Articles in your inbox
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
 The true story of Feud: Capote vs. The Swans
The true story of Feud: Capote vs. The SwansIn depth The writer's fall from grace with his high-flying socialite friends in 1960s Manhattan is captured in a new Disney+ series
By Adrienne Wyper, The Week UK Published
-
 Scottie Scheffler: victory for the 'pre-eminent golfer of this era'
Scottie Scheffler: victory for the 'pre-eminent golfer of this era'Why Everyone's Talking About Masters victory is Scheffler's second in three years
By The Week Staff Published
-
 Crossword: April 20, 2024
Crossword: April 20, 2024The Week's daily crossword
By The Week Staff Published
-
 Dengue hits the Americas hard and early
Dengue hits the Americas hard and earlySpeed Read Puerto Rico has declared an epidemic as dengue cases surge
By Peter Weber, The Week US Published
-
 How happy is Finland really?
How happy is Finland really?Today's Big Question Nordic nation tops global happiness survey for seventh year in a row with 'focus on contentment over joy'
By Harriet Marsden, The Week UK Published
-
 How Tehran became the world's nose job capital
How Tehran became the world's nose job capitalUnder the radar Iranian doctors raise alarm over low costs, weak regulation and online influence of 'Western beauty standards'
By Harriet Marsden, The Week UK Published
-
 Africa's renewed battle against female genital mutilation
Africa's renewed battle against female genital mutilationUnder the radar Campaigners call for ban in Sierra Leone after deaths of three girls as coast-to-coast convoy prepares to depart
By Harriet Marsden, The Week UK Published
-
 Argentina: the therapy capital of the world
Argentina: the therapy capital of the worldUnder the radar Buenos Aires natives go hungry to pay for psychoanalysis, amid growing instability, anxiety – and societal acceptance
By Harriet Marsden, The Week UK Published
-
 Does declining birth rate spell doom for Britain?
Does declining birth rate spell doom for Britain?Today's Big Question Ageing population puts pressure on welfare state, economy and fabric of society, while fertility is rising on populist agendas
By Harriet Marsden, The Week UK Published
-
 How a new blood test could revolutionise sepsis diagnosis
How a new blood test could revolutionise sepsis diagnosisThe Explainer Early results from ongoing trial suggest faster identification of deadly condition is possible
By The Week Staff Published
-
 Kush: the drug destroying young lives in West Africa
Kush: the drug destroying young lives in West AfricaThe Explainer There has been a sharp rise in young addicts in Sierra Leone, Guinea and Liberia
By Flora Neville, The Week UK Published