Blood donation rules: who can donate?
The NHS warns that donation levels are worrying low, but are their donor restrictions too extensive?
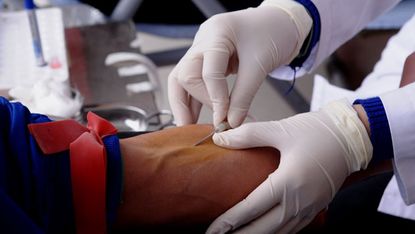
The NHS is facing calls to lift restrictions on blood donation amid a crisis in the number of people giving blood in the UK.
The health service describes blood donation as an “essential part” of the healthcare system and although more than a quarter of Britons will require a blood transfusion in their lifetime, just 4% of the population donate regularly.
135,000 new donors are needed every year to ensure it has the right mix of blood groups to meet patient needs now and in the future, yet a combination of misconceptions, stringent restrictions and changing lifestyles have seen donor levels plummet in recent years.
Subscribe to The Week
Escape your echo chamber. Get the facts behind the news, plus analysis from multiple perspectives.

Sign up for The Week's Free Newsletters
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
From our morning news briefing to a weekly Good News Newsletter, get the best of The Week delivered directly to your inbox.
Why have blood donations fallen?
Overall, the number of new blood donors in the UK has dropped by more than 40% in the last decade.
Health officials point to a number of different factors, including an increase in foreign travel and busier lifestyles. “People are working longer hours, commuting further, spending more time online and have less time of their own,” says Jon Latham, assistant director for donor services and marketing at NHS Blood and Transplant. “Travel to more exotic places, tattoos and investigations such as endoscopy are [also] becoming more common and these lead to short-term deferrals from donation.”
Common misconceptions
A survey conducted last year by the NHS revealed a number of widespread misconceptions about blood donation, The Guardian reports. Nearly half of the respondents said they think the NHS asks friends and family to donate when a patient needs blood, which is untrue.
“Worryingly, the survey also revealed that one in eight people wrongly believe ‘synthetic blood’ is created to meet the needs of national demand, such as in vampire TV drama, True Blood,” the newspaper reports.
Are some groups under-represented among donors?
Donations of blood and stem cells within black and Asian communities has reached “crisis levels”, according to a government review published last year.
Only 69% of patients in general can find suitable blood matches from strangers. However, this figure drops to just 20% if you are a patient from a black, Asian or ethnic minority background.
Despite this, less than 5% of donors who gave blood in the last year were from black, Asian and ethnic minority communities, despite making up 14% of the population, says the NHS.
Blood conditions such as thalassaemia and sickle cell disease most commonly affect people within these communities. Patients with these disorders need regular blood transfusions to stay alive and benefit from donations from those with a similar ethnic background.
Thalassaemia mainly affects people with a south-Asian or Mediterranean heritage, while sickle cell disease mainly affects black people. The NHS estimates that 1,000 people in the UK have thalassaemia and between 13,000 and 15,000 have sickle cell disease.
Rarer forms of O negative, A negative and B negative blood are also constantly in short supply, says Cosmopolitan.
Sky News says that “demand is growing so rapidly, it is estimated that in the next year alone, 27,000 extra blood donors are needed from these backgrounds to meet patients' needs”.
Lindsay Johns, who presented The Black Donor Crisis on BBC Radio 4 in June, says there are a myriad of factors why BAME blood donation is so low, including: more pressing concerns for working-class people of colour, a residual distrust of “white institutions”, and cultural and religious traditions.
To address these concerns, MPs have said a cultural shift is needed around donation and called for public awareness campaigns in the media to help change perceptions around donation. It also recommended schools introduce teaching about donation as part of the national curriculum with the aim of providing children with “myth-busting tools that are often vitally needed in BAME communities”.
What about men?
Another demographic drop has occurred in male donors. Wired says the number of men giving blood in England has dropped by almost 25% in the last five years, “and when they do sign up to give blood, men are less likely than women to actually deliver on the pledge”.
Of all the new donors who registered during 2018, only half as many men went on to donate compared to women, meaning there are now 100,000 more women on the blood donor register than men.
“And this is a big problem” says Wired, “because men are particularly useful blood donors”.
Larger average size means men can donate more frequently. “Men also tend to have fewer antibodies in their blood – as women often produce them during pregnancy – making men’s blood less likely to cause reactions in patients, and more suitable for creating blood products, including platelets and plasma transfusions given during surgery or cancer treatment.”
So who can give blood?
According to the NHS, 135,000 new donors are needed every year to ensure it has the right mix of blood groups to meet patient needs now and in the future.
The majority of the British population is able to donate blood, says the NHS. As long as the donor is fit and healthy, weighs over 7st 12lb (50kg) and is between 17 and 66, they are typically allowed to give blood. Male donors are allowed to donate about 470ml (just under a pint) every three months and women at four month intervals.
http://www.blood.co.uk/donor-information/
And who can't?
There are several exceptions. As well as those with existing medical conditions, the following people may not be allowed to donate blood:
- Anyone who has travelled to certain countries outside of the UK within the past six months
- Anyone who has had a tattoo, piercing or acupuncture in the past four months
- Men who have had sex with men (with or without a condom) in the last three months
- Anyone who has had sex with a sex worker in the last year
- Anyone who has sex with someone who has been sexually active in parts of the world where Aids/HIV is very common in the last year
- Anyone on antibiotics
- Pregnant women and anyone receiving IVF treatment
- Anyone who has been to the dentist in the last week
Hasn’t the ban on gay men giving blood been lifted?
With blood in short supply, many argue that some of these restrictions could be lifted. The most controversial of these has been the long-running ban on sexually active gay men giving blood, with many calling it prejudiced.
The restrictions were first introduced in the 1980s at the height of the Aids crisis in a bid to prevent the risk of HIV contamination, the BBC says.
Since then there has been a slow but steady relaxing of restrictions. Lifetime bans were lifted in 2011, allowing gay men to donate if they abstained from sex for a year.
The NHS had previously defended this decision, saying there is a “window period” after HIV infection during which it is impossible to detect the virus. With a one-year ban, there is a risk of infection in every 4.38 million donations, but if that were lifted, the risk would increase to one in every 3.48 million donations.
However, last November, the year-long prohibition period was further reduced to allow gay men to give blood three months after sex.
“The rule is in line with improved NHS testing measures, which can establish whether someone has a blood infection such as HIV, hepatitis B, hepatitis C or syphilis within that time period,” says The Independent.
Liam Beattie, Blood Donations Policy Lead at Terrence Higgins Trust, said the charity was pleased that the law had been swiftly brought into force, adding that the new rules will enable more people to give blood.
“We hope this paves the way for more progress as further evidence becomes available, and we’re now urging the government to continue to regularly review the deferral periods in line with the latest evidence” he said.
Create an account with the same email registered to your subscription to unlock access.
Sign up for Today's Best Articles in your inbox
A free daily email with the biggest news stories of the day – and the best features from TheWeek.com
-
Why is Tesla stumbling?
In the Spotlight More competition, confusion about the future and a giant pay package for Elon Musk
By Joel Mathis, The Week US Published
-
 How Taylor Swift changed copyright negotiations in music
How Taylor Swift changed copyright negotiations in musicunder the radar The success of Taylor's Version rerecordings has put new pressure on record labels
By Theara Coleman, The Week US Published
-
 Job scams are increasingly common. Here's what to look out for.
Job scams are increasingly common. Here's what to look out for.The Explainer You should never pay for an application or give out your personal info before being hired
By Becca Stanek, The Week US Published
-
 Martha's Rule: patients given right to urgent second opinion
Martha's Rule: patients given right to urgent second opinionThe Explainer Hospitals in England will launch new scheme that will allow access to a rapid treatment review
By Richard Windsor, The Week UK Published
-
 The contaminated blood scandal
The contaminated blood scandalThe Explainer Widely regarded as the worst treatment disaster in the history of the NHS, the public inquiry is due to publish its report in May
By The Week UK Published
-
 Can Britain's dental crisis be fixed?
Can Britain's dental crisis be fixed?The Explainer New proposals include more money for dentists working in under-served areas
By Richard Windsor, The Week UK Published
-
 Babylon Health: the failed AI wonder app that 'dazzled' politicians
Babylon Health: the failed AI wonder app that 'dazzled' politiciansThe Explainer Demise of UK tech start-up is a cautionary tale for politicians seeking quick fixes to complicated problems
By The Week UK Last updated
-
 Surgery faces ‘MeToo moment’ as female staff assaulted while operating
Surgery faces ‘MeToo moment’ as female staff assaulted while operatingTwo-thirds of women surgeons claim to have been sexually harassed and a third alleged assaults
By Chas Newkey-Burden Published
-
 What does UK’s first womb transplant mean for future of fertility?
What does UK’s first womb transplant mean for future of fertility?Today's Big Question Procedure could be offered more widely including to transgender people
By Chas Newkey-Burden Published
-
 The NHS plan for virtual wards to beat winter crisis
The NHS plan for virtual wards to beat winter crisisfeature Patients with respiratory infections to be given wearable devices that allow doctors to monitor them at home
By The Week Staff Published
-
 The NHS at 75: can it make it to 100?
The NHS at 75: can it make it to 100?feature The NHS is facing almost unprecedented challenges, but support for the institution remains strong with the public
By Sorcha Bradley Published